Osteoarthritis (OA) of the knee is a common degenerative joint disease that we see at Cheltenham Podiatry. It is characterised by the breakdown of cartilage in the knee joint. Here’s an overview of its pathology, classification, and management:
Causative factors:
The causes of knee osteoarthritis can vary, but they generally involve a combination of genetic, biomechanical, and environmental factors. Here are some common causes:
- Age: Aging is the most significant risk factor for knee osteoarthritis. As people age, the cartilage in their joints naturally wears down, increasing the likelihood of osteoarthritis development.
- Joint Injury or Trauma: Previous knee injuries, such as ligament tears, meniscal tears, or fractures, can predispose individuals to develop osteoarthritis later in life. Injury-related changes in joint mechanics and instability contribute to cartilage degeneration.
- Obesity: Excess body weight places increased stress on the knee joints, accelerating cartilage degeneration and worsening symptoms of osteoarthritis. Obesity is a significant risk factor for the development and progression of knee osteoarthritis.
- Genetics: Genetic factors play a role in determining an individual’s susceptibility to osteoarthritis. Certain genetic variations may influence the structure and integrity of joint tissues, affecting their ability to withstand mechanical stress and repair damage.
- Biomechanical Factors: Abnormalities in joint alignment, such as bow-leggedness (varus deformity) or knock-knees (valgus deformity), can increase the risk of osteoarthritis by altering joint mechanics and distributing uneven loads across the joint surfaces.
- Occupational or Recreational Activities: Repetitive stress on the knees from activities such as squatting, kneeling, or lifting heavy loads can contribute to cartilage wear and tear over time, increasing the risk of osteoarthritis.
- Joint Overuse: Activities that involve high-impact or repetitive movements, such as jumping, can accelerate cartilage degeneration and contribute to the development of knee osteoarthritis, especially when performed excessively or without proper rest and recovery.
- Other Medical Conditions: Certain medical conditions, such as rheumatoid arthritis, gout, or metabolic disorders, can predispose individuals to osteoarthritis or exacerbate existing symptoms.
- Gender and Hormonal Factors: Women are more likely than men to develop knee osteoarthritis, particularly after menopause, suggesting that hormonal factors may play a role in disease onset and progression.
Understanding these underlying causes can help guide preventive measures and targeted interventions to reduce the risk of knee osteoarthritis and manage symptoms effectively.
Pathology:
- Cartilage Degeneration: The cartilage covering the ends of the bones gradually deteriorates, leading to roughened surfaces and decreased shock absorption. This leads to an increase in inflammatory proteins in the joint.
- Bone Changes: Over time, the underlying bone may undergo changes such as osteophyte (bone spur) formation, cysts, and sclerosis (increased bone density).
- Synovial Inflammation: Inflammation of the synovial membrane may occur due to increase in the inflammatory proteins, leading to pain and swelling.
- Muscle Weakness: Surrounding muscles may weaken due to disuse or pain inhibition, further contributing to joint instability.
- Ligament and Meniscus Changes: Degenerative changes can affect the ligaments and menisci within the knee joint, increasing instability.
Classification:
- Primary vs. Secondary OA: Primary OA occurs due to aging and wear-and-tear on the joint, while secondary OA may result from factors like joint injury, obesity, or genetics.
- Location: OA can affect different compartments of the knee joint, including the medial (inner) compartment, lateral (outer) compartment, or patellofemoral joint (between the kneecap and thigh bone).
- Severity: OA can be classified based on the severity of symptoms and radiographic findings, ranging from mild to severe. Stage 1 to Stage 4
Management:
- Lifestyle Modifications: Weight management, regular exercise (including low-impact activities like swimming or cycling), and avoiding activities that exacerbate symptoms can help manage OA.
- Physical Therapy: Strengthening exercises, stretching, pilates , yoga and a planned structured rehabilitation program ( eg Glad program) and modalities like heat or ice therapy can improve joint function and reduce pain.
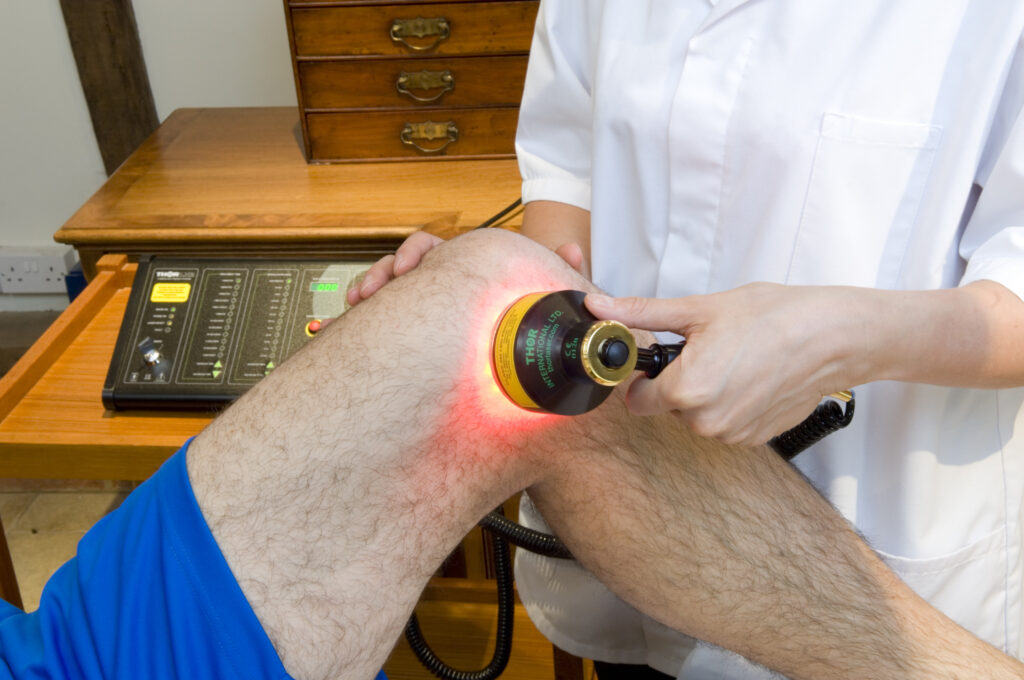
- Laser– Photobiomodulation can be used as an adjunct therapy. It is non invasive, painless and no adverse affects. It works via absorption of various wavelengths of light by chromophores in the cells, that act to improve cellular function, has anti-inflammatory affects, reduces pain and improves function.
- Medications: Over-the-counter pain relievers or nonsteroidal anti-inflammatory drugs (NSAIDs) can help alleviate pain and inflammation temporarily but are not a good long term solution due to adverse effects. In some cases, corticosteroid injections can provide short-term relief, however recent research implicates it in progressing the cartilage degeneration at a faster rate. .
- Bracing and Assistive Devices: Knee braces and orthotic devices can provide support and stability to the joint, reducing pain and improving function.
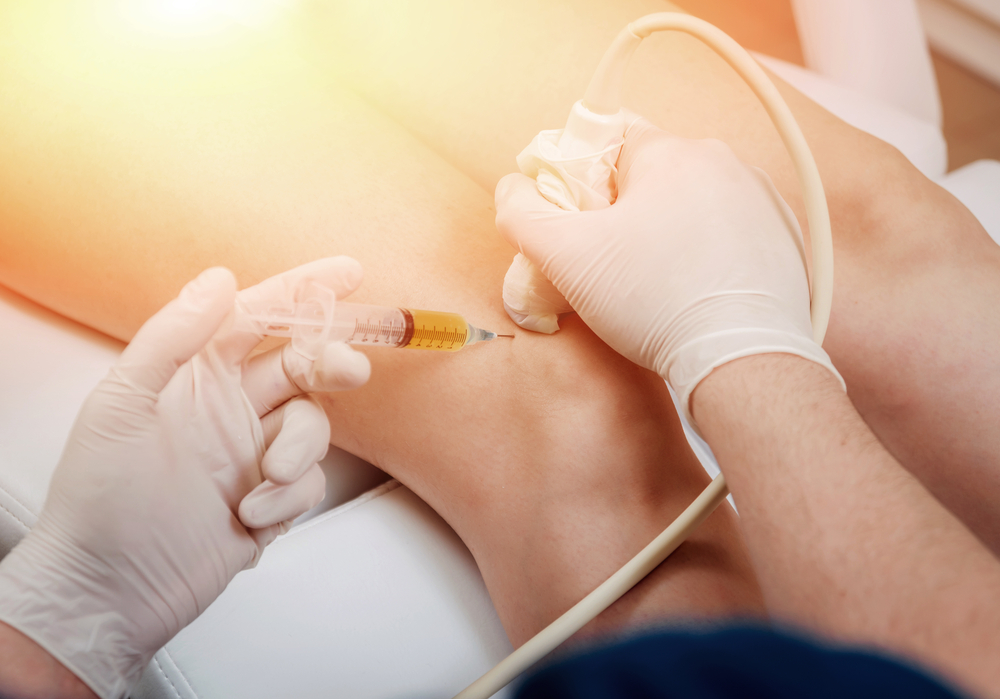
- Injections: Hyaluronic acid injections (viscosupplementation) have been utilised, Prolotherapy ( medical grade Glucose ) and Platelet-rich plasma (PRP) injections are also becoming increasingly popular.
- Prolotherapy is a medical grade glucose injection, that acts as a temporary irritant. It leads to a release of growth factors that can reduce inflammation and pain. It has minimal adverse effects, and it is injected via ultrasound guidance for accurate placement.
- Evidence has been accumulating of PRP’s potential in providing sustained pain relief, and slowing of the disease progression. This is due to increased understanding of the nuances of appropriate dosing requirements. That is, the appropriate platelets numbers, and appropriate white blood cell/ leucocyte profile. Recent research points to approx 8-10 billion platelets required per knee injection, with a high concentration of Mononuclear cells ( lymphocytes and Monocytes ), these are anti inflammatory and minimal concentration of Polymorphonulcear cells (basophils , eosinophils, neutrophils), which are pro inflammatory.
- Surgery: In cases of severe OA that do not respond to conservative treatment and injection therapy , surgical options such joint replacement (total or partial) may be considered.
Individualised plans should be tailored to each patient’s symptoms, functional limitations, and preferences, with the goal of reducing pain, improving function, and optimising quality of life.
Here at Cheltenham Podiatry, we provide a tailored treatment plan for the individual. This will encourage and improved lifestyle modifications, carry out biomechanics adjustments, rehabilitation program and injection therapies as appropriate. Jacqueline has been carrying out injection therapies knee arthritis for over 10 years and has continuously updated and fine tuned her skills. Our injection are ultrasound guided, this allows for precise and accurate placement and thus better outcomes.
We aim to get you moving again, and doing the things you love!
Chu, J., Duan, W., Yu, Z. et al. Intra-articular injections of platelet-rich plasma decrease pain and improve functional outcomes than sham saline in patients with knee osteoarthritis. Knee Surg Sports Traumatol Arthrosc 30, 4063–4071 (2022). https://doi.org/10.1007/s00167-022-06887-7
Rabago, D., Patterson, J. J., Mundt, M., Kijowski, R., Grettie, J., Segal, N. A., & Zgierska, A. (2013). Dextrose prolotherapy for knee osteoarthritis: a randomized controlled trial. Annals of family medicine, 11(3), 229–237. https://doi.org/10.1370/
Latest News
Treatment for peripheral Neuropathy with B12 Injections
Peripheral Neuropathy is changes to the sensory nerves and in[…]




